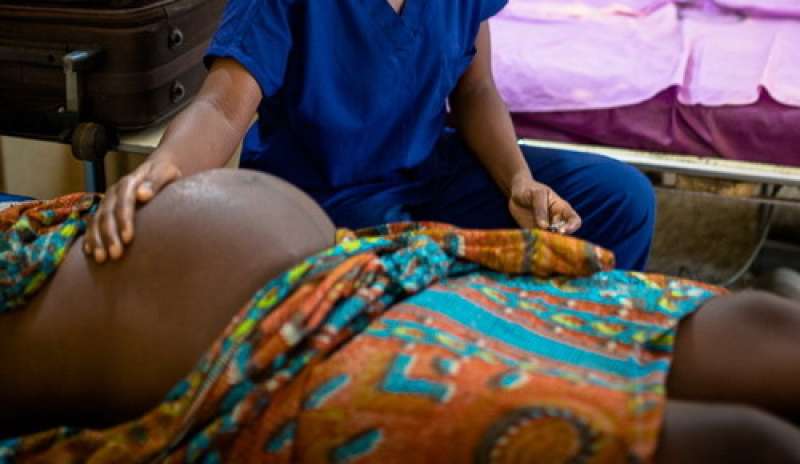
An effective response to Ebola in Sierra Leone is hampered by the same issues that make it the most dangerous country in the world to deliver a baby, writes Professor Peter Piot in the Financial Times.
An effective response to Ebola in Sierra Leone is hampered by the same issues that make it the most dangerous country in the world to deliver a baby, writes Professor Peter Piot in the Financial Times.Written in collaboration with Dr Mohamed Yilla, Country Director of MamaYe! Sierra Leone, the article explores the silent epidemic of maternal mortality; one that inspires less horror but claims many lives. The article was published on July 29th 2014 in the Financial Times online and printed in the newspaper on July 30th.Peter Piot is Director of London School of Hygiene and Tropical Medicine, one of the Consortium partners driving forward the work of MamaYe. He was the founding Executive Director of UNAIDS and was the co-discoverer of the Ebola Virus in 1976. Read the full article below.Financial Times/London: The Ebola virus, which has struck more than 1,000 people in three African countries since May, can kill as many as nine-tenths of the people it infects. It is one of the most deadly agents of disease, and an even more potent inspiration of horror.What begins as muscle pain or a headache soon becomes a burning fever. The virus affects the brain: victims often come over in a fixed and vacant gaze, and some experience psychosis. In the late stage of the disease, blood vessels burst and there is heavy bleeding, including from the eyes and mouth. A few droplets of an infected person’s blood contain enough virus particles to claim the next victim. Infections commonly occur among those who have handled the dead.When I first encountered Ebola at close quarters in 1976, it was an unknown virus that had yet to acquire its fearsome name. A blue Thermos flask arrived at the Antwerp laboratory where I was a young researcher, containing blood from a woman in what was then Zaire who had died from an unidentified haemorrhagic fever. Travelling to the affected region, I witnessed the suffering the virus causes in the impoverished communities where it most easily spreads. (We later relinquished our samples to a US lab with elaborate safety equipment.)The outbreak in West Africa has affected countries where the disease has not been seen before. Infections have been found in at least 60 places. Heightened action is needed, with better co-ordination. Frightened and therefore hostile communities must be persuaded that doctors are there to help.Equally important is what happens when the emergency subsides and media attention drifts away. In the four decades since the virus was discovered, successive crises have attracted the attention of the global media and western donors. But as soon as people stop falling ill, the money disappears. Little is invested in preventing the next epidemic.Time and again I have witnessed fitful concern give way to long spells of indifference in which epidemics are incubated. Without routine surveillance, outbreaks can go unnoticed for months. Without proper training, health workers do not follow procedures to prevent contamination. Without adequate water and sanitation infrastructure, disease spreads. All of this must be remedied if epidemics are to be controlled and experimental treatments properly evaluated. Such systems take time to build. But the attention generated by an Ebola outbreak is inevitably shortlived.Too often we focus on the illnesses we currently find most horrific, not those that cause most sufferingThe same goes for the silent epidemics that inspire less horror but claim many more lives. One is maternal mortality. In high-income countries people have forgotten what a risky business it is to have a baby without proper medical care. Sierra Leone, one of the countries affected by the Ebola outbreak, also happens to be the riskiest place in the world to bear a child. My colleague Mohammed Yilla of the MamaYe programme in Sierra Leone estimates that about 460 women have perished there from pregnancy-related causes since the start of the epidemic in May, roughly double the number of Ebola fatalities. But these women’s deaths will not be officially recorded – a sign that priorities lie elsewhere.Why the apparent indifference? Perhaps because maternal mortality is not contagious, or is not regarded as gruesome. Perhaps because it is something that happens only to women – although the tragedy is surely shared. Perhaps because, too often, we focus on the illnesses we currently find most horrific, not those that cause most suffering.Maternal mortality and other scourges like it may not fit the typical public health professional’s definition of an emergency. The monthly toll does not readily fall – there has been little improvement in Sierra Leone since the beginning of this decade – but nor does it rise. An infectious disease, by contrast, can kill at a faster rate with every week that it is allowed to spread. But they are emergencies all the same.There is no contradiction between fighting maternal mortality and preventing the next Ebola epidemic. Both can be stopped with the same kind of long-term investment in health infrastructure. These investments do not involve cutting-edge technology, although they are logistically complex. They will take time, but they will also endure.The writer is director of the London School of Hygiene and Tropical Medicine and former executive director of UNAidsTo access the original article please visit the Financial Times.Find out what is happening in Ghana here.